






 |
||||
 |
 |
 |
 |
 |
 |
||||
|
Gracias, Doctores!
 For a Johns Hopkins pediatric medicine team, a mission to Peru was a crash course in diagnosing and treating tropical disease. But the larger lessons the doctors and nurses learned on the trip were about poverty and suffering — and their own capacity to relieve them.
Story and photos by
Gary Logan |
|

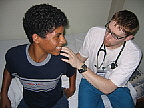

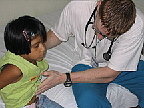
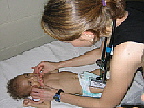
|
A group of American physicians, residents, and
nurses makes its way across the dusty courtyard of a
temporary clinic set up on the edge of town in Chulucanas.
Led by Johns Hopkins pediatric emergency medicine physician
Karen Schneider, the team has come to this northwest corner
of Peru to spend two weeks tending to sick children, many
of whom have never seen a doctor before. This will be some of the toughest medicine the Americans have ever practiced — and for some, the poorest patients they've seen. Outside the clinic gate, children and their families, dressed in their Sunday best, wait for the doctors in a long line. Surprisingly, the atmosphere is festive. As the team walks by, the families erupt in applause. Though other American medical missions have come to Chulucanas in the past, this is the first time in 30 years that pediatricians have visited the town, the local bishop explains as he greets them. "You come to dare to touch the leper," he says. "When you touch the children, you touch the entire community." This morning, and in the days ahead, the team — which includes Patrick Wilson and Megan Partridge, both pediatric residents at Hopkins, and Shannon Mitchell, a Hopkins pediatric nurse — will diagnose and treat tropical diseases they rarely if ever run up against in the States: cholera, hepatitis-A, malaria, typhoid, and yellow fever, among others. And they'll do so without labs, X-rays, or the array of antibiotics that have been integral to their previous practice. Schneider, who is a Sister of Mercy as well as an emergency department doc, has been running medical missions for six years, to places like Belize, Guyana, Haiti, and Peru. She became involved in this kind of work as a fourth-year medical student on a trip to Guyana, where she spent two weeks in a village fighting a malaria epidemic. Since then, she's traveled up and down the Amazon, treating children with cleft palates, infectious and parasitic diseases, leprosy, and severe wasting. When Schneider joined the Hopkins faculty in 2002, Children's Center Director George Dover suggested that she turn her volunteer missions into an elective for pediatric residents. Since then, she has led missionary teams on eight trips to Third World countries, treating some 10,000 children. On the first day in Peru, the team met with Bob Gilman, a researcher from Johns Hopkins Bloomberg School of Public Health, who has been fighting Peru's health problems for 20 years. (Gilman spends about half of each year working in Peru, and the other half teaching at Hopkins.) The country is plagued by malaria, malnutrition, maternal deaths, and a vicious cycle of parasitic infections. Underlying those problems, Gilman told them, are pervasive poverty — more than 50 percent of the country's population lives below the poverty level — two decades of terrorism that have taken some 70,000 lives, and corrupt governments that have neglected the people and their living conditions. More than 25 percent of urban residences and more than 90 percent of rural residences lack potable water and sewage treatment, resulting in high death rates from infectious diseases. Here, health care is provided by so-called "barefoot doctors," local people with limited medical training who staff one-room clinical outposts serving 10,000 people each. It is one of the frustrations the group will realize in the days ahead — they can treat the disease but not the cause. "It's not all medical," Wilson says. "It's social, economic, developmental, infrastructure. What do these kids need? Clean food and water, as well as access to health care."
The day the team arrived at the clinic in
Chulucanas, Schneider gave the group a M*A*S*H-like prep
talk. Her instructions are antithetical to their training.
At Hopkins, a thorough pediatrician obtains history upon
history — behavioral, developmental, family, feeding,
neonatal, and prenatal. A physical exam means a litany of
measurements — from blood pressure and respiration to
height and weight and head circumference — and body
parts to check — abdomen, chest, extremities, eyes,
ears, nose, mouth, throat, lymph nodes, and skin. Here, a
"medical history" needs to be limited to the chief
complaint. |
| Families line up at the clinic in Chulucanas, waiting to be seen by the American pediatricians. |
 At the clinic, local health volunteers will weigh the children, check their skin for scabies, give them a pill to rid their intestines of worms, treat their teeth with fluoride, and send them to an exam room. Then the residents will examine the patients, making do with what they have. There is no lab or X-ray, though they can order blood work and imaging in Piura, a large city 30 miles west of Chulucanas. On exam, Schneider tells the team, check the lungs, ask the patient to breathe, and look for nasal flaring and head bobbing, which would indicate respiratory illness. Do a quick skin check for impetigo and ringworm lesions. Call for the other doctors if the case is unusual or unclear. Practice your own way but be brief. "I don't want to sound like an HMO," Schneider says, "but you have about five minutes with each child." Partridge, a third-year resident, first sees a 5-year-old boy with a sore throat. She feels his neck for swollen lymph nodes, then looks inside at large, inflamed tonsils. The child's mother says he has suffered four infections like this over the past year. Does he need surgery? Not necessarily, Partridge answers through a translator. The tonsils are not obstructing his airway. She prescribes an antibiotic and tells the mother to take him to the local hospital if the infections continue.
Next comes the boy's 8-year-old sister, who is experiencing
headaches so severe she vomits. Has she seen an eye doctor?
asks Partridge. No, not in two years, says the mother, who
cannot afford the three soles — about $1 — for
an eye exam. Partridge writes a prescription for Ibuprofen
and directs the family to the pharmacy across the
courtyard. There, between filling prescriptions and
administering nebulizer treatments, Mitchell applies
permithren cream head to toe on children with scabies to
kill the mites, knowing that in this environment it's only
a matter of time before they return. |
| "It's not all medical," Patrick Wilson says of the problems his patients face. "What do these kids need? Clean food and water, as well as access to health care." |
In the neighboring consultation room, Wilson, a second-year
resident, examines a 12-year-old girl with a painful lump
in her left breast. Has she bumped into anything? he asks
the mother in Spanish. Si. Breast tissue is more sensitive
at the onset of menstruation, Wilson explains. This is not
a tumor but a fibroma, fat tissue necrosis, he adds. If the
breast becomes inflamed, red, and hot, come back. As the girl leaves, Wilson begins to take the history of a 14-month-old boy with bloody stools. He feels the child's neck for swollen lymph nodes, then squeezes the ends of the infant's fingers, looking for signs of anemia. Giardia, he tells the mother as he calculates a prescription for zinc based on the infant's weight. Nothing unusual so far — what Wilson has seen, he could see at Hopkins. But next door, Partridge is facing her first challenging case, a 3-year-old cerebral palsy patient with seizures so severe that over time he had bitten off his lower lip. A group of surgeons, including a plastic surgeon, will be coming the week after the pediatricians leave, Partridge tells the mother as she fills out a surgical consult. A random mix of cases follows, from bellyaches and headaches to hernias and vitamin deficiencies. "I saw two hepatitis-A cases," Wilson says during the team's lunch break. "I'm a fish out of water." Malnutrition underlies the bellyaches, dehydration the headaches, Schneider explains. The pain goes away after they eat and drink, then returns when they are hungry again. She adds that on the following day, she'll be offering a lecture on hepatitis-A, a viral infection of the liver caused by exposure to water, fruits, and vegetables contaminated by feces.
After lunch, Schneider greets 9-month-old Oscar in her exam
room, turning on her chair to face him, opening herself to
the chubby child and blocking his path at the same time,
giving him nowhere else to go. "Bueno, bueno. You
have not missed a meal," she tells him. He's been coughing
a lot, his mother says, as Schneider places her stethoscope
on his chest. "His lungs are absolutely clear. He's fine,"
says the pediatrician, sending mother and child on their
way only minutes after they entered the room. Sometimes a
mother makes up symptoms to have the child checked out, to
see if anything really is wrong, Schneider explains. |
| Mitchell, Wilson, and Partridge after a full day at their clinic in the Andes. |
 Wilson stops by holding hospital X-rays of a 14-year-old
who has been suffering low back pain since a wall fell on
him a year ago. Schneider and Wilson step out to the
courtyard and hold the black film against the sun. The
pelvis looks OK, they agree, and prescribe Ibuprofen for
the child's pain. Meanwhile, back inside, Partridge is
looking into the eyes of a 6-year-old with headaches,
searching with an otoscope for any signs of intracranial
pressure, such as blurring of the optic disc or speckles in
the back of his eye, but sees none. Growing pains, she
tells the mother. This patient is followed by a 4-year-old
girl with white spots on her chest. Not to worry, Partridge
tells the mother as she writes a prescription for a topical
lotion. Then the little girl stands on her toes and
Partridge leans over to receive her first kiss,
beso, something all the team members will experience
repeatedly in the days ahead. In her travels as a
volunteer, Schneider has seen mothers so grateful they've
kissed the tops of her feet.
Wilson stops by holding hospital X-rays of a 14-year-old
who has been suffering low back pain since a wall fell on
him a year ago. Schneider and Wilson step out to the
courtyard and hold the black film against the sun. The
pelvis looks OK, they agree, and prescribe Ibuprofen for
the child's pain. Meanwhile, back inside, Partridge is
looking into the eyes of a 6-year-old with headaches,
searching with an otoscope for any signs of intracranial
pressure, such as blurring of the optic disc or speckles in
the back of his eye, but sees none. Growing pains, she
tells the mother. This patient is followed by a 4-year-old
girl with white spots on her chest. Not to worry, Partridge
tells the mother as she writes a prescription for a topical
lotion. Then the little girl stands on her toes and
Partridge leans over to receive her first kiss,
beso, something all the team members will experience
repeatedly in the days ahead. In her travels as a
volunteer, Schneider has seen mothers so grateful they've
kissed the tops of her feet.Wilson's next case is 5-year-old Jesus, "the miracle child," his parents call him because he is the only one of their three children to have survived. Wilson writes a prescription for his stomach pain and sore throat. His final patient, his 38th of the day, is a 9-year-old boy with, of all things, anxiety about school exams. At dinner they review their first day. Everybody had bone pain and bellyaches, diarrhea and headaches. Mitchell noted that she had filled prescriptions for 80 patients in the pharmacy, plus nebulizer and scabies treatments for another dozen. The volume of cases was something new. "You're forced to practice differently," Wilson says. "It's really fast — boom, boom, boom — and you wonder, 'Am I giving optimal care seeing this many patients?'" "It makes you think out of the box and use what you have," says Partridge, "which is real limited."
After two days in Chulucanas, where the team would
treat a total of 400 patients, they head for the Andes to
set up a clinic for three days. There, in Frias, life is
even simpler. But with less running water and sanitation,
the villagers' health problems are greater, which the team
sees firsthand soon after loud speakers announce the
arrival of the "miracle workers from America." Now whole
families enter their consultation rooms, holding triage
cards with stick-man drawings marking the number of hours
— from one to seven — families had walked from
the surrounding hills to reach the clinic. |
| In lieu of state-of-the-art medical equipment, Partridge uses her eyes, ears, and hands to make a diagnosis. |
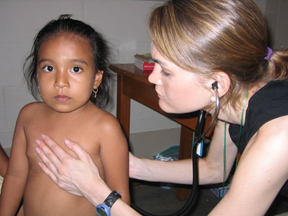 "Gastrito," Wilson says, feeling a girl's belly,
then pointing to his own stomach to explain her pain. Next
a 3-year-old boy who has suffered scabies the past two
years. Endemic in developing countries because of crowding
and poor sanitation, scabies mites living on the surface of
the skin spread from person to person by contact and
persistent scratching. The result is impetigo, marked by
white, thread-like inflammatory nodules on the skin. So
severe is the itch that some children scratch through the
skin to bare bone.
"Gastrito," Wilson says, feeling a girl's belly,
then pointing to his own stomach to explain her pain. Next
a 3-year-old boy who has suffered scabies the past two
years. Endemic in developing countries because of crowding
and poor sanitation, scabies mites living on the surface of
the skin spread from person to person by contact and
persistent scratching. The result is impetigo, marked by
white, thread-like inflammatory nodules on the skin. So
severe is the itch that some children scratch through the
skin to bare bone."Respiro," Wilson instructs the boy as he holds his stethoscope against his chest. The mother says her son pulled a foot-long worm out of his anus. The daily double — scabies and worms. Indeed, almost every child he and Partridge examine has parasites from drinking unfiltered water and eating vegetables from gardens fertilized with human feces. "'Treat as parasite' is becoming a dictum," Wilson says.
There are the unpredictable cases, too, a young boy with
the hallmark spots of hepatitis, but with no jaundice, no
enlarged liver. He vomits after every meal, which concerns
Partridge the most. She calls in Wilson, who, pointing to
low platelets, suspects vessel vasculitis, a post-infection
process related to hepatitis. After leafing through the
Red Book, the diagnostic bible of infectious
diseases, Partridge agrees. Thanks for the consultation,
she tells Wilson. They seem quite comfortable, like veteran
detectives on a case, collaborating this way, and they're
doing more of it as the cases become more mysterious. Now,
in the Andes, they find what they may have been searching
for when they signed up for Schneider's tropical medicine
course — patients who would push the envelope of
their diagnostic skills, cases that appeared to have no
answers. And in many cases, they would find, there were
none. |
| "You say to yourself, 'If I wasn't there, the kid would have died,'" says Karen Schneider. "That changes you." |
For Partridge, one of the most challenging cases is a
patient with neurocysticercosis, caused by ingestion of the
pork-tapeworm and marked by cysts in the brain that can
lead to headaches, infections, seizures, and death. She can
treat the child with antiparasitics, but unless she
administers IV steroids at the same time, there is a risk
of brain swelling and death. What the child needed was a
neurologist in Piura, but the family, who had walked six
hours through the mountains to see Partridge, had no money.
Then there was the child with opsoclonus-myoclonus —
known as "dancing eyes-dancing feet" — a rare
neurologic disorder characterized by a trembling gait and
rapid eye movements. An MRI could determine the cause
— possibilities include a brain tumor or a viral
infection — and how to treat it. But there's only one
MRI in Peru, in Lima, a city light-years away from this
poor family in the Andes. One case especially would stay
with her more than the others, a 4-year-old who had been
hit in the eye with a stick. With no money for treatment,
the child lost his vision and his eye grew so grotesque
that he wore a baseball hat low and looked away to avoid
embarrassment. As the mother broke down in tears, Partridge
tried to reassure her that her son might be able to get a
prosthetic eye, though she knew it was unlikely: "It was so
sad. I had to take a break before I went on to the next
patient." For Wilson, the take-home cases are an immune-deficient young girl oozing pus from her eye and missing parts of her skull because of a rare syndrome, and an abused 4-year-old who had been locked up like an animal, who screamed and scratched her face incessantly, who wouldn't walk. "I'm sitting here almost in tears, asking myself, What can you do with this kid who was healthy but severely abused?" Wilson says. "She needs brain imaging, therapy, social work, but there are no resources." They would face such cases for another two days in Frias and for another week in the hamlets surrounding Chulucanas. In all, during their two-week stay, the team saw 2,268 patients. They diagnosed eight serious heart murmurs, including a 10-year-old girl with a ventricular septal defect, a hole in her heart, whose father planned to sell the family goat so he could afford a cardiac echo for her in Lima. They detected hernias in 52 patients, including five boys with scrotums halfway down their thighs. On her next trip, Schneider hopes to bring a pediatric surgeon to treat them.
Clinical successes? Yes, the team agreed, but there were so
many children who couldn't be diagnosed, let alone
treated. |
| For many of the children in Frias, this was their first-ever visit to a doctor. Back at Hopkins, Mitchell says, "The faces of the children stay with you." |
 "That was the hard thing about all this," Partridge says,
"informing the parents of your concerns and then being
unable to provide the diagnostic testing and care we have
back home."
"That was the hard thing about all this," Partridge says,
"informing the parents of your concerns and then being
unable to provide the diagnostic testing and care we have
back home.""We were putting band-aids on this huge gaping wound," says Wilson. But they helped whom they could. What they received in return was intense field training in hands-on medicine, the chance to learn how to diagnose through history and exam alone. Ingrained in the experience is what you feel, see, and hear, not what a lab or radiology report tells you. Back at Hopkins, adjusting to a lower volume of patients and a much larger volume of clinical notes, Partridge and Wilson realize that on the side of a mountain, in Frias, they had never felt so focused, so in charge before. "It makes you more reliant on your exam," Wilson says. "Over there, we listen, oscillate, palpate. We do that here at home, but it's not definitive — the radiographic study is." Even with a diagnosis, treatment is limited. Everyone is immuno-compromised, but there's no immunology service to refer them to — or any other specialty, for that matter. Surgeons rotate in and out from time to time, but not often. And with no money or mode of transportation, the families have nowhere else to go. "You say to yourself, 'Oh my God, I went through all that training to save one kid on the mountain. If I wasn't there, the kid would have died,'" says Schneider. "That changes you." Much about a medical mission — about caring for an extremely poor population — changes a person. It was only after returning to the States and settling back into life at Hopkins that the impact of this searing experience began to sink in for the team. As they reflected on the patients they could not fix, they asked themselves, Why is there this suffering? Why them, not me? As Schneider says, it's not like you go under a mango tree, do a clinic, and walk away free and clear: "You have to ask why, but there are no answers." "You continue to wonder what happens to the kids after you leave," Partridge says. "The faces of the children stay with you," Mitchell adds. Those faces were new windows into the human psyche, spirit, and soul. Over and over again, team members saw how the families coped with terminal illnesses, how strongly the parents wanted the best for their children, yet how little they had to help them. "When you see the suffering that's out there, it kind of reminds you of why you went into medicine," Wilson says. "This is why, to help people. This is where you're supposed to be. You can bring that home with you." Gary Logan is associate director of communications and public affairs at Johns Hopkins Children's Center. |
 |
|
 The Johns Hopkins Magazine |
901 S. Bond St. | Suite 540 |
Baltimore, MD 21231
The Johns Hopkins Magazine |
901 S. Bond St. | Suite 540 |
Baltimore, MD 21231Phone 443-287-9900 | Fax 443-287-9898 | E-mail jhmagazine@jhu.edu |
|