|
Getting a straight answer
|
|
When Michael Ain was 19, he underwent a
surgical procedure known as an osteotomy to straighten his
bowed legs. It involved breaking and resetting the legs. The
procedure caused Ain a good deal of pain, and he lay in a
body cast for several months.
A wrestling injury prompted Ain's surgery, but doctors
recommend the procedure to many achondroplasts with bowed
legs to reduce their chances of arthritis.
Now that he is an orthopedic surgeon, Ain suspects that this
medical premise may not apply to all achondroplastic dwarfs,
about half of whom have the condition. "I think many
[achondroplasts] do not need any type of treatment," he
says.
The link between bowing and arthritis is based on research
involving patients of average stature, Ain notes. Bowing may
increase pressure at the knee joint, setting the stage for
arthritis. But because achondroplasts have shorter limbs,
they may not have the same degree of risk, suggests Ain.
To test this theory, he and biomedical engineer Edmund Chao
are creating a biomechanical computer model of
bowleggedness. Ain is also conducting clinical studies in
achondroplasts older than 40 to see whether the amount of
arthritis the patients have correlates with their degree of
bowleggedness.
--MH
|
|
Ain did well at Albany and decided while he was there that he
wanted to become a pediatric neurosurgeon. He was an avid
woodworker and had always enjoyed working with his hands. And he
liked the immediate gratification such surgery provided. Ain
applied to 14 residency programs, had nine interviews, and was
rejected by every program. He then applied to nine or 10 general
surgery residencies, including some "bottom of the barrel
programs" to which a candidate with inferior credentials would
have been admitted. Again, they turned him down.
The gatekeepers of the residency programs were blunt. "Every
place one guy said, 'You can't do it physically' or 'Patients
won't respect you,'" recalls Ain.
Ain spent the next year doing a pediatrics residency at the
University of California at Irvine. Though he enjoyed working
with children, he still yearned to be in the operating room. So
Ain wrote to John Hall, a renowned pediatric orthopedic surgeon
at Children's Hospital in Boston, who had done surgery to
straighten Ain's bowed legs when Ain was 19. When Ain was in
medical school, he had done a rotation at Children's under Hall's
supervision. In his letter to Hall, Ain asked what his chances
would be of getting into an orthopedic surgery residency. Hall
was encouraging, and Ain applied to two residencies. He was
considering a third, but the chairman at that program told him,
"There's no way you're going to get in. You should be quite happy
doing pediatrics," Ain recalls.
But the chairman at Albany Medical College did not see it that
way. Richard Jacobs, who is now retired, told Ain, "If your
record is as good as everybody else's, you'll get in. It doesn't
matter whether you're 4 feet 3 inches or 6 feet 3
inches. We will take you." After examining Ain's record, Albany
accepted him.
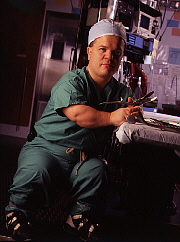
In entering the ranks of orthopedic surgery, Ain was indeed
standing certain assumptions on their heads. Of all the
specialties, orthopedics has a machismo reputation--not without
some justification. It takes a fair amount of strength to push
and pull fractured bones back into place. When a patient has
dislocated a hip, for instance, an orthopedist has to lift the
patient's leg and push against muscle and soft tissue to force
the hip back into the socket. The tools of orthopedic surgery are
bold and serious affairs. An orthopedic cart parked in the
Hopkins operating suite resembles a medieval hardware store:
drills, saws, reamers, mallets, hooks, rods, and screws--tools
for cutting bone, reducing fractures, drilling holes for
screws.
During his five-year residency at Albany, Ain proved he could do
the job, says Allen Carl, an associate professor of surgery at
Albany who was one of Ain's mentors. "He's just a wonderful
person who exudes the positive," notes Carl.
While at Albany, Ain also began dating a nurse named Valerie
Frinks, who, at 5 feet 6 inches, is of average stature. They
married and now have a 2-year-old daughter, Alexa. Their daughter
is a little person, says Ain, and he does not want to discuss her
size in any more detail than that. "She is the most delightful,
beautiful person," he adds.
At first, Ain thought he might become a hand or joint surgeon. He
never considered specializing in bone disorders such as
achondroplasia. "It's the last thing in the world I wanted to do
because it's like looking in the mirror every day," he says.
That feeling changed one day in the operating room, when Carl
mentioned to Ain that he had read a newspaper article about a
couple from southern California who had an achondroplastic
daughter. The parents were worried about the limitations their
child would face. (After all, notes Ain, "Where do you see most
little people? On TV, at the circus.") But the father had been
encouraged when he met a physician at a party who was an
achondroplast. If this man could become a physician, the father
reasoned, then his daughter could have many opportunities in her
life.
Ain suddenly realized that he was the physician at that
party.
|